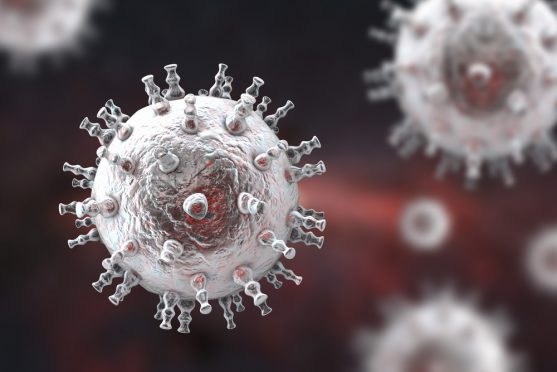
HIV stands for human immunodeficiency virus. It infects the immune cells of the body, and over time can result in acquired immunodeficiency syndrome (AIDS) which is a chronic, progressive, and life-threatening condition. AIDS is the most advanced stage of HIV infection.
HIV is a major global health issue. HIV causes disruption of the body’s immune system, thereby making a person more vulnerable to opportunistic infections or diseases, and some cancer types. The virus destroys and impairs the functions of immune cells. infected individuals, over the time, become immunodeficient.
The risk of HIV-infected people developing cancers at a younger age is higher than in the general population.
Globally, about 38 million people are infected with HIV, and among them, 2.1 million HIV patients are in India. HIV prevalence among adults (aged 15-49) is an estimated 0.2%.
Although HIV-related cancers are more common globally, there is not much information about HIV-related cancers in Indians.

The link between HIV and cancer
The connection between HIV and cancer is not completely understood. Multiple factors may contribute to the increased incidence of cancer in patients infected with HIV. These include immunosuppression, direct effects of the HIV virus itself, co-infection with other oncogenic viruses like HHV8, HPV, EBV, HBV HCV and environmental factors.
Immunosuppression makes a person vulnerable to infection by the viruses that are known to cause cancers. In addition, chronic antigenic stimulation, inflammation, and cytokine dysregulation are some factors that may contribute to lymphoma and other types of cancers.
Infection with HIV may sensitize cells to the oncogenic effects of environmental stimuli such as tobacco. For example, there is a significant increase in the risk of lung cancer in HIV-infected individuals. Although there is a higher incidence of tobacco use in this population, the risk of lung cancer remains approximately three-fold higher compared with the general population after adjusting for smoking status. Colon, breast, and prostate cancer are a common type of cancers in aged HIV-positive patients.
The common types of HIV-related cancers
Cancers in HIV or AIDS patients are usually defined in two ways. Cancers that occur more commonly or frequently in HIV or AIDS patients are known as AIDS defining cancers, such as Kaposi sarcoma, aggressive B-cell non-Hodgkin lymphoma, and cervical cancer.
In addition to these cancers, HIV infected people are at increased risk of several other cancers, which are collectively referred to as non-AIDS defining cancers.
In persons with HIV, all cancers except Kaposi’s sarcoma, aggressive B-cell lymphoma, and invasive cervical cancer are considered non–AIDS defining cancers. The most common AIDS related cancer type in India is non-Hodgkin’s lymphoma.
-
Kaposi’s sarcoma
The presence of Kaposi sarcoma indicates that the HIV infection is in the advanced stages. Current evidence suggests that HIV infected people have 500 times higher risk of developing Kaposi sarcoma compared to the general population.
Kaposi sarcoma is a type of cancer that mostly develops in the cells lining the blood and lymph vessels. It usually appears as a tumour on the skin or the mucosal surfaces. These tumours may also develop in other parts of the body, such as the lungs and the digestive tract.
Causes and symptoms
Kaposi sarcoma is caused by a virus called human herpesvirus 8 (HHV-8). Healthy people usually have a strong immune system, and hence can fight HHV-8 infection. whereas, in immune-compromised conditions, such as HIV or AIDS, HHV-8 infects the cells and multiplies abnormally and has the potential to trigger kaposi’s sarcoma through an unknown mechanism.
Kaposi sarcoma usually appears as purple, red, or brown coloured lesions on the skin, usually on the legs or the face. These lesions don’t cause any symptoms, but may become a cosmetic concern. In rare cases, these lesions may cause painful swelling of the legs and feet.
Diagnosis
Kaposi sarcoma is usually diagnosed by a biopsy, in which a small sample of tissue is collected from the suspicious skin lesion and examined in the laboratory to look for any abnormalities. If internal Kaposi sarcoma is suspected, then, faecal occult blood test, chest X-ray, bronchoscopy, upper endoscopy, and colonoscopy are recommended.
-
Non-Hodgkin’s lymphoma
The risk of non-Hodgkin’s lymphoma in HIV-infected people is 12 times more than in healthy people. Similar to Kaposi sarcoma, non-Hodgkin’s lymphoma is also a condition that indicates the transition of HIV to the advanced stage.
Causes and symptoms
Non-Hodgkin’s lymphoma occurs due to the overproduction of abnormal lymphocytes in the body. Gradually, these abnormal lymphocytes continue to grow and divide, thereby getting accumulated in the lymph nodes. Therefore, swollen and painless lymph nodes in the neck, armpits, or groin region are one of the most common symptoms of non-Hodgkin’s lymphoma.
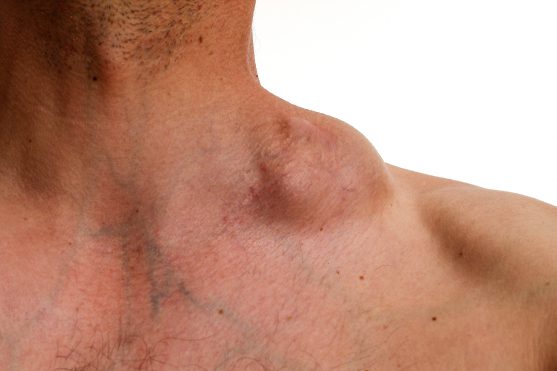
Other symptoms of non-Hodgkin’s lymphoma include the following:
- Pain or swelling in the abdomen
- Anaemia
- Chest pain
- Cough
- Trouble breathing
- Fever
- Itchy skin
- Loss of appetite
- Night sweats
- Unexplained weight loss
- Weakness and fatigue that doesn’t go away
Diagnosis
A physical examination is initially done to determine the size and condition of the lymph nodes. Additionally, laboratory tests, such as a blood test are done to rule out other conditions.
Imaging tests, such as X-rays, CT scan, MRI scan, and PET scan, lymph node biopsy, Bone marrow aspiration and biopsy are done to determine the stage and extent of cancer.
-
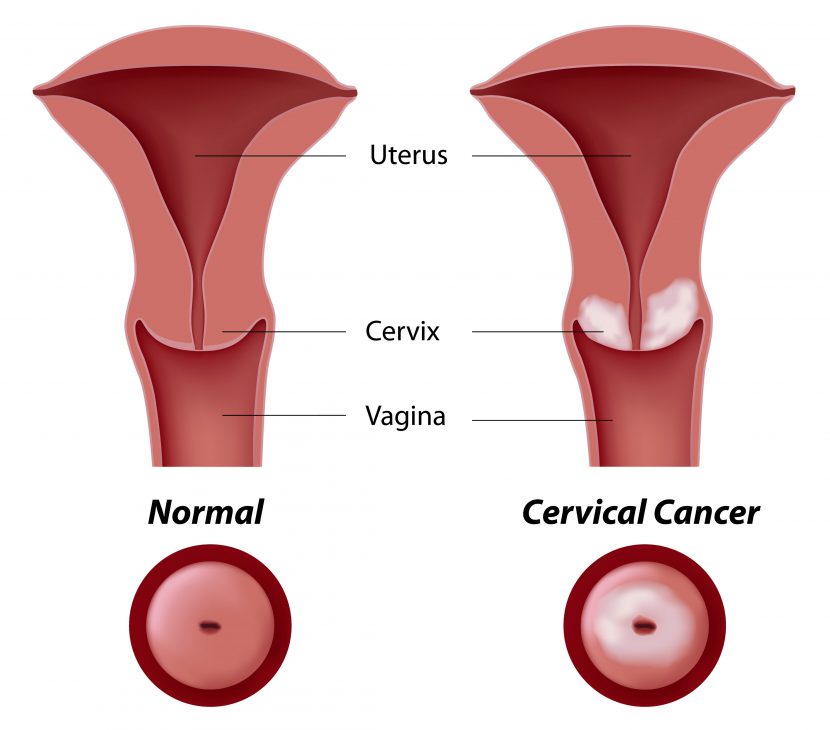
Cervical cancer
Women with HIV infection have three times higher risk of being diagnosed with cervical cancer than their healthy peers.
Causes and symptoms
Although the exact reason for cervical cancer is unknown, scientists believe it occurs due to DNA mutations in the cells lining the cervix. Also, some factors such as human papillomavirus (HPV) infections, becoming sexually active at a young age, smoking, and a weakened immune system may also increase the risk.
Cervical cancer may not cause any signs or symptoms during the early stages. However, in some cases, it may typically cause the following symptoms:
- Bleeding after douching and sexual intercourse
- Bleeding after menopause
- Irregular or abnormal bleeding between periods
- Longer or heavy menstrual bleeding than usual.
- Pain during intercourse
- Watery, bloody vaginal discharge that may be heavy and have a foul odor
- Unexplained persistent pelvic pain or severe back pain
Diagnosis
A routine pelvic examination is done to look for any unusual changes. In addition, the overall health of the patient, medical and personal history is evaluated.
To confirm the diagnosis some laboratory tests, such as a blood test including routine blood work up and renal function tests and liver function tests, colposcopy, biopsy, imaging tests like CT scan, and MRI scan,PET CT are recommended to determine the extent of disease spread.
Other HIV related cancers
HIV infected people are at a higher risk of developing the following non-AIDS defining cancers (NADCs) when compared to non-HIV infected people:
- 19 times higher risk of anal cancer
- 3 times higher risk of liver cancer
- 2 times higher risk of lung cancer
- 2 times higher oral and oropharyngeal cancer
- 8 times more likely to develop Hodgkin’s lymphoma
Risks factors for cancer in HIV patients
The compromised immune system is the major risk factor for cancer in HIV patients. Also, the progression of cancer cells is much faster in HIV infected people than in HIV uninfected people.
HIV-infected persons are more likely to be infected with the oncogenic viruses (cancer causing viruses) than people in general population like Kaposi sarcoma associated herpes virus(KSHV), Human herpes virus(HHV-8) that can cause kaposi sarcoma and some subtypes of lymphoma. Epstein Barr Virus (EBV) which can cause some subtypes of Hodgkins Lymphoma and Non Hodgkins Lymphoma, Human papilloma viruses(HPV) which can cause cervical cancers, anal caner, and oropharyngeal, penile , vaginal and vulval cancer, Hepatitis B virus(HBV) and Hepatitis C virus (HCV), which both causes liver cancer.
In addition to this, the traditional risk factors that contribute to the development of cancers in HIV are Heavy alcohol consumption and tobacco Smoking.
Measures to reduce the risk factors
The following measures may help in reducing the risk of HIV-related cancers:
- Using combination antiretroviral therapy (CART): According to HIV treatment guidelines, taking CART therapy reduces the risk of Kaposi sarcoma and non-Hodgkin lymphoma. Also, it improves the overall survival rates.
- Knowing the status of viral hepatitis: HIV-infected people are more prone to infections, especially viral infections. They also have a higher risk of liver cancer. So, checking their hepatitis status regularly and taking both HBV suppressing agents and CART therapy can help in lowering the liver cancer risk.
- Screening for cancers: Screening is always a key to diagnose and treat cancers at an early stage. HIV infected patients should undergo regular screening to check for AIDS-related cancers and other cancers too. For example screening for cervical cancer using pap smear cytology.
- Smoking cessation: HIV infected people are at a higher risk of lung, oral, and other cancers associated with smoking. Therefore, smoking cessation could be a great way to reduce its risk.

Avoiding/limiting alcohol intake may help lower the risk of some cancers.
Some types of cancers linked with HIV and AIDS are caused by viruses that can be spread through sex, so using safer sexual practices may also help protect against those cancers.
Being physically active and maintaining a healthy weight, and eating a balanced nutritious diet, may help lower a person’s risk of cancer.
Treatment for HIV and cancer
Those with HIV already have a weak immune system even before they start cancer therapy. This factor makes cancer and HIV treatment more complex. Therefore, several factors, such as the type of cancer, stage of cancer, immune system function, response to treatment, and overall health status of the patient is considered while treating cancer coexisting with HIV.
The cancer treatment is usually the same in HIV uninfected and HIV infected people. Chemotherapy, radiation therapy, immunotherapy, targeted therapy, and surgery are the standard treatment options for cancer.
The anti-HIV treatment should also go hand in hand with the cancer treatment for better outcomes. HIV patients who are on anti-HIV drugs can get a full dose of chemotherapy and other treatment options to improve overall survival rates.
However, certain modification in the drug dose and regimen might be required depending upon the state of the immune system of HIV infected people.
The outcome of treatment in HIV positive patients are worse compared with HIV negative patients and HIV positive patients present late and are less likely to complete oncological treatment.
Treating AIDS-defining cancers
Anti-HIV therapy is an important part of treating AIDS-defining cancers.
Kaposi sarcoma: Anti-HIV therapy is recommended in HIV infected people diagnosed with Kaposi sarcoma. Anti-HIV therapy is sufficient treatment in non-visceral disease.
For visceral disease where there are several internal lesions, chemotherapy is recommended. For locally symptomatic disease, radiation therapy may be introduced.
Non-Hodgkin lymphoma: It is of several types, but the type, which is linked to HIV is the fast-growing one and needs to be treated with intensive chemotherapy.
Usually, the treatment for non-Hodgkin lymphoma is the same as in individuals with HIV uninfected non-Hodgkin lymphoma patients. However, chemotherapy must be given with caution and the blood counts must be monitored regularly during the treatment course.
Cervical cancer: The management is similar to that in non HIV infected women with cervical cancer. The immune status must be checked regularly along with proper treatment for HIV infection.
Women with advanced cervical cancer may not have a good response to radiation therapy alone. Chemotherapy is recommended in women with advanced or recurrent cervical cancer. Irrespective of the CD4 status, anti-HIV therapy must be given to improve the treatment outcomes in HIV infected women.
Women with HIV infected cervical cancer must be monitored regularly to ensure the cancer doesn’t recur.