Radiation therapy uses high-energy X-rays or other particles to kill tumor cells. It may be used to slow or stop the growth of the tumor. It is typically given after surgery and possibly along with chemotherapy. A doctor who specializes in giving radiation therapy to treat a tumor is called a radiation oncologist. A radiation therapy regimen, or schedule, usually consists of a specific number of treatments given over a set period of time.
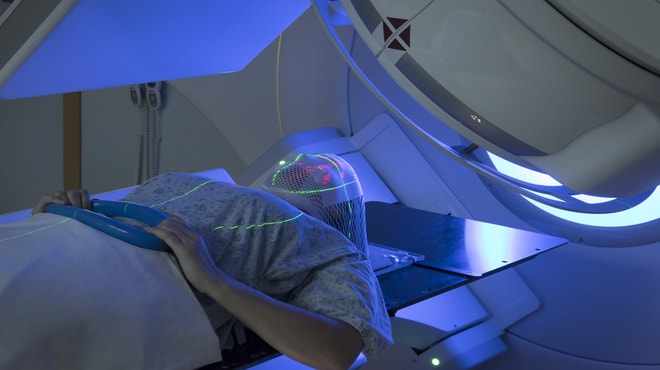
The most common type of radiation treatment is called external-beam radiation therapy, which is radiation given from a machine outside the body. It can be directed at the tumor in the following ways:
-
Conventional radiation therapy.
The treatment location is determined on anatomy of the landmarks and X-ray images of them. The dosage usually depends on the grade of the tumor. In certain instances of tumor in the brain, this technique is quite appropriate.
-
3-dimensional conformal radiation therapy (3D-CRT).
A 3-dimensional model of the tumor and healthy tissue surrounding the tumor is created on a computer, using images from CT and MRI scans, a. This model is then utilized to target radiation beams directly at the tumor, sparing the healthy tissue from high doses of radiotherapy.
-
Intensity modulated radiation therapy (IMRT).
IMRT is a type of 3D-CRT that has greater access to a tumor. It can deliver higher doses of radiation to the tumor in order to kill it while giving less to the surrounding healthy tissue.
-
Proton therapy.
Proton therapy is a type of external-beam radiation therapy that makes use of protons rather than X-rays. At high energy, protons can kill tumor cells. Proton beam therapy is typically used for tumors when less radiation is needed because of the vital normal structures adjacent to the tumor. For instance, the tumors that have grown into nearby bone, such as the base of skull, and those near the optic nerve.
-
Stereotactic radiosurgery.
Stereotactic radiosurgery uses a single, high dose of radiation. This is shot directly to the tumor and not healthy tissue. It works best for a tumor that is only in 1 area of the brain and certain non-cancerous tumors. It can also be used when a person has more than 1 metastatic brain tumor. There are many different types of stereotactic radiosurgery equipments, a few of which are:
- A modified linear accelerator is a machine. It creates high-energy radiation by using electricity to form a stream of fast-moving subatomic particles.
- A gamma knife. It concentrates highly focused beams of gamma radiation on the tumor.
- A cyberknife. It is a robotic device used in radiation therapy to guide radiation to the tumor target, more often in the brain, head, and neck regions.
-
Fractionated stereotactic radiation therapy.
Radiotherapy that is delivered with stereotactic precision but broken across several days of doses called fractions and given over several weeks, in contrast to the 1-day radiosurgery. This procedure is used for tumors located close to sensitive structures, like the sensory nerves or the brain stem.
When radiation treatment is given using implants, it is called internal radiation therapy or brachytherapy. Radiation oncologists may use high dose rate (HDR), low dose rate (LDR), and pterygium-specific forms of brachytherapy. HDR involves radioactive seeds precisely positioned in the body for as little as a few minutes to a half hour. It’s often an outpatient procedure. LDR is an inpatient procedure to implant radioactive cesium seeds, either for a short time or permanently. Brachytherapy can also be used to treat pterygium, an eye condition.
With these different options of treatment, doctors strive for precision and reduction in radiation exposure to the surrounding healthy brain tissue. Depending on the size and location of the tumor, side-effects, and the patient’s preference, the radiation oncologist may recommend any of the kinds of radiation techniques. In certain situations, a combined techniques may work best.
Read more on the side effects of radiotherapy in the treatment of brain tumor.



