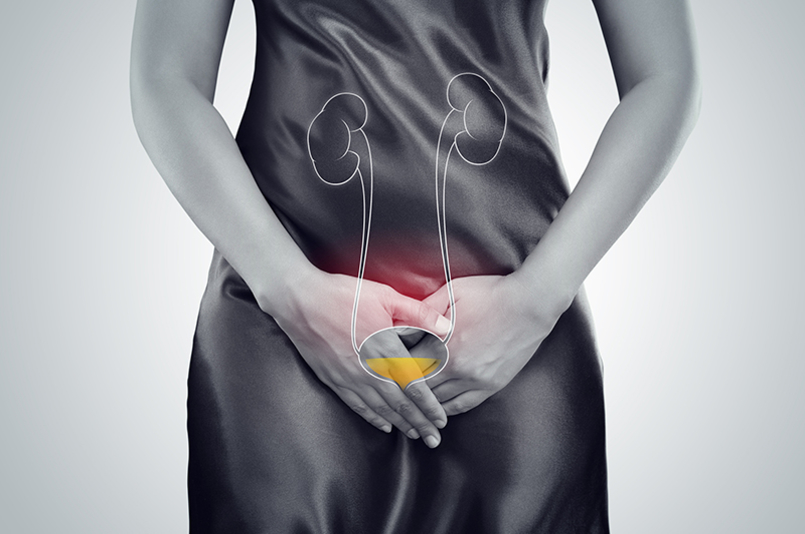
The urinary bladder is a hollow muscular sac in the pelvis just above and behind the pelvic bone. It has flexible and muscular walls that stretch to contain urine and squeeze it to send it out of the body. Urine is liquid waste made by the pair of kidneys, which is then carried to the bladder by channels called ureters. Urination happens when the muscles in the bladder contract. Urine passes out of the bladder through a tube called the urethra. This article focuses on the types of and treatment options available for bladder cancer.
What is bladder cancer
Bladder cancer occurs when the cells of the bladder begin to grow uncontrollably. As the number of cells increases, they form a tumor and eventually spread to other parts of the body. Also, read more on the stages.
The causes are not definite, but genetic history, genetic mutations due to the use of tobacco or exposure to chemicals are important risk factors. Moreover, smokers are more likely to develop bladder cancer than nonsmokers. Other risk factors are:
- Bladder defects at birth
- Side-effects of chemotherapy and radiation therapy
- Chronic bladder infections and irritations
- Exposure to chemicals, including aromatic amines and arsenic in water
- Low fluid consumption
- Family genetic history of bladder cancer
- Being male and white
Types of bladder cancer
There are different types of bladder cancer. However, the most common are:
Urothelial carcinoma (transitional cell carcinoma)
This is by far the most common type. This form starts in the urothelial cells, which line the inner lining of the bladder. These cells also line parts of the urinary tract. TCC can occur in the lining of the kidneys and the ureters. Anyone who receives a diagnosis of TCC undergoes an assessment of the whole urinary tract.
TCCs are prominent and slow to spread, which depends on whether they remain in the lining (epithelium) of the bladder, or even if they have spread further into the lamina propria or muscle layer. In other words, TCCs become harder to treat as they become obtrusive. They are of two kinds:
- Papillary carcinomas develop as slight projections from the inner surface of the bladder towards the hollow focus. They are non-intrusive papillary malignant growths. The low-grade forms have favorable results with a less probability of danger.
- Level carcinomas develop on the internal layer of the bladder cells and are known as level carcinoma in situ.
There are other less common varieties of bladder cancer, and they are as follows:
Squamous cell carcinoma:
About 1 or 2 percent of bladder malignancies are of this type. They occur in the squamous cells, the thin lining cells that usually make up the outside of the skin. They are malignant and intrusive. The lining epithelium of bladder, at places, changes into squamous type in some chronic infections that predispose to cancer.
Adenocarcinoma:
Approximately 1 percent of bladder diseases are of this type. They occur in the bodily fluid discharging organs found in the bladder. It resembles colon cancers, and most forms are intrusive in nature. Incidentally, developmental abnormalities of urinary bladder sometimes add to the risk of developing the disease.
Small cell carcinoma:
Fewer than 1 percent of bladder cancer is of the variety. Primarily, it originates at the nerve-like cells called neuroendocrine cells. They spread rapidly and require treatment with chemotherapy.
Sarcoma:
This is the most remarkable variety of bladder cancer that starts in the muscle cell of the bladder.
Symptoms of bladder cancer
Early signs of bladder cancer are to do with urinary problems. The following are the symptoms of bladder cancer in brief:
- Blood in the urine
- Pain or discomfort during urination
- Frequent urination
- Feeling the need to urinate throughout the night
- Feeling the need to urinate but not being able to pass urine
- Lower back pain on one side of the body
Stages of bladder cancer
If the diagnosis is confirmed, further tests are recommended, and they include CT and MRI scans, chest X-rays, and bone scans.
Staging determines how far cancer has spread and the treatment options best to kill cancer cells.
Cancer cells, is stage 0, occur on the outer surface of the inner lining of the bladder, and it is called ‘carcinoma in situ.’
In stage 1, cancer cells occur within the inner lining but has spread to the lamina propria but not to the muscular wall
During stage 2, the tumor has spread to the muscular wall but has not spread from the bladder
Cancer has invaded through the wall to the tissue surrounding the bladder, including potentially the prostate, uterus, or vagina or lymph nodes, when it has reached stage 3.
In stage 4, cancer has invaded pelvic bones/ abdominal wall or has spread to other bones or other organs such as the lungs or liver.
Treatment of bladder cancer
The primary treatment modalities for bladder cancer are surgery, chemotherapy, and radiation therapy. Oncologists may advise treatment individually or in combination to treat the tumor more effectively. Besides, the treatment also depends on the location and stage of cancer, the patient’s overall health, age, and preferences.
Surgery
Surgical treatment for bladder cancer is available at all stages of bladder cancer:
A transurethral resection (TUR) is advised at the initial suspicion of bladder cancer. A surgeon removes the abnormal tissues and sends it across for histopathological examination. Incidentally, it provides information about the approximate depth of the tumor and helps decision making.
Moreover, radiation waves help kill the remaining cancer cells. Sometimes a surgical procedure to remove the bladder may be required if the tumor does not respond well to radiation or is unlikely to return. Also, read more on surgery for bladder cancer.
Chemotherapy
Chemotherapy uses drugs to target and kill cancer cells or to shrink tumors, so non-invasive surgery is possible. It is administered in many cycles, and after a period of treatment, the body is allowed to rest and recover. Furthermore, read chemotherapy in the treatment of bladder cancer.
Radiation
Radiation uses high energy waves to damage cancer cells and kills them by preventing them from multiplying or dividing. It is a local treatment modality just as surgery is. In recent times, the use of radiation as a solitary procedure instead of combination therapy with chemos. Read more on the treatment of bladder cancer with radiation therapy.
Follow-up for bladder cancer
Regular monitoring of bladder cancer after the treatment regime is finished important as the chances of recurrence are very high. Check-ups need to be one every 3 to 6 months. Sometimes bladder cancer does not go away and becomes chronic.
Diagnosis of bladder cancer
After a review of the symptoms, medical history, and a physical examination, the doctor confirms the diagnosis with a series of tests and procedures:
Cystoscopy:
A cystoscope is a narrow tube that contains a camera and lighting system that is inserted into the bladder through the urethra under local anesthesia. The doctor examines the inside of the urethra and the bladder using the cystoscope. Moreover, the device collects cell samples or a biopsy for testing.
Imaging tests
Finally, the following imaging tests help confirm the diagnosis and determine whether cancer has spread to other parts of the body:
- Pyelogram: This is a contrast dye injected into the bladder either by a vein or by a direct catheter. The color outlines the bladder and nearby organs, making any tumors visible on the X-rays.
- CT scan: This helps determine the shape, size, and position of any tumors that might be in the bladder, kidney, or ureters.
- Ultrasound and sonography: There determine the size and spread of the tumor.
Urine tests:
Urine tests spot traces of cancer cells. There are three primary types:
In a urine cytology, the sample of the urine is under examination, but negative results do not always guarantee the absence of cancer.
Urine cultures monitor urine samples in a growth medium for signs of bacterial growth. For instance, if bacteria appear to prevail, the diagnosis may show an infection instead of cancer.
In urine tumor marker tests, the tumor marker tests examine urine samples for specific substances that indicate abnormality; these tests happen alongside urine cytology.
Read more here.
Related Posts: