Radiation therapy or radiotherapy uses high-energy rays to kill cancer cells by preventing their growth and rapid division. It consists of local treatment that delivers waves within the radiation field either externally or internally. External radiation delivers high-energy rays directly to the cancer from a machine outside the body. Internal radiation, or brachytherapy, involves the implantation of a small amount of radioactive material in or near the cancer.
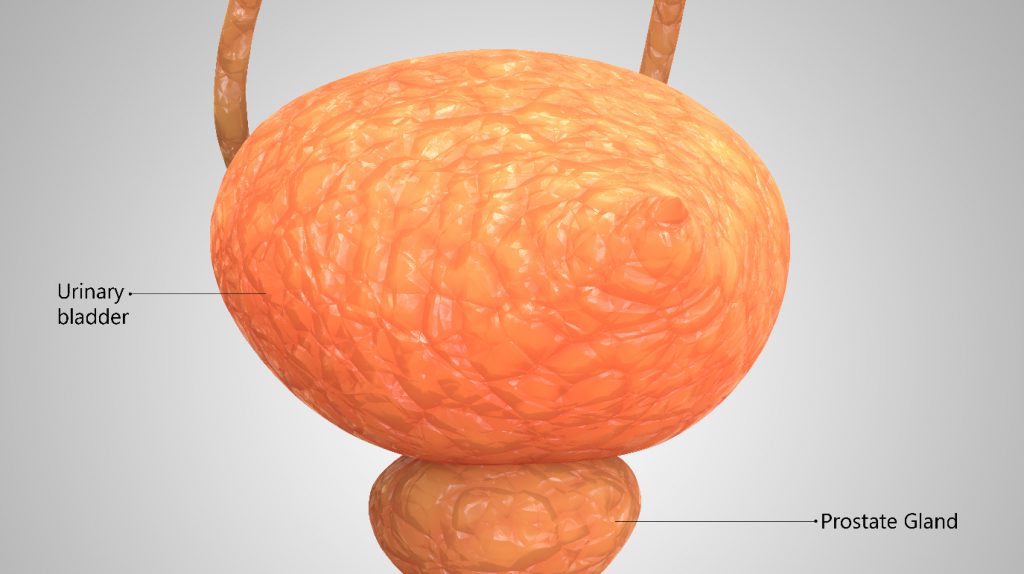
Before treatment of bladder cancer with radiotherapy, simulation, a planning process helps make careful measurements to find exact angles for administration and the right dosage. It may include imaging tests like CT or MRI scans.
During simulation, patients lay on a table somewhat similar to the one in a CT scan. Adjustments of height and rotation around a central axis is possible. The ‘simulator’ machine is a machine whose dimensions and movements closely match that of an actual linear accelerator. The simulator lets the radiation oncologist and technologists treat the tumor by projecting an image of it.
The simulator room is periodically darkened while the treatment fields are being set and temporary marks may be made on the patient’s skin with the help of markers. The radiation oncologist is aided by one or more radiation technologists and often a dosimetrist, who performs calculations necessary in the treatment planning. The simulation may last anywhere from 15 minutes to an hour or more, depending on the complexity of the plan.
Furthermore, read about the side effects of radiotherapy in the treatment of bladder cancer.
Palliative Radiation
Palliative therapy helps reduce the symptoms of cancer and ultimately improve the patient’s quality of life. For some patients with advanced bladder cancer, radiation therapy may help shrink cancer lumps and relieve cancer symptoms.
Administration of radiation therapy today for bladder cancer happens through linear accelerators. These accelerators produce high energy external radiation beams that penetrate the tissues and deliver the radiation dose into deeper areas. These modern machines and other state-of-the-art techniques significantly reduce side effects. Moreover, they help improve the ability to deliver a curative radiation dose to cancer-containing areas and minimizing the radiation dose to normal tissue.
X-rays representing the treatment fields follow the positioning of the treatment fields. In most centers, the oncologist marks the patient multiple places which punctate the radiation field. These marks look like pin pricks and they are subject to renewal each day.
The administration of radiation treatment happens in a room separate from the simulation room. The treatment plans and treatment fields that result from the simulation session are transferred over to the treatment room. The latter contains a linear accelerator that focusses on a patient table similar to the one in the simulation room. However, treatment starts only when the field and calculations are accurate.
Doctors may prescribe radiation therapy in combination with chemotherapy for treatment of patients with stage II-III disease or recurrent cancer. However, radical cystectomy remains the primary modality for the treatment of stages II bladder cancer and treatment of stage III bladder cancer