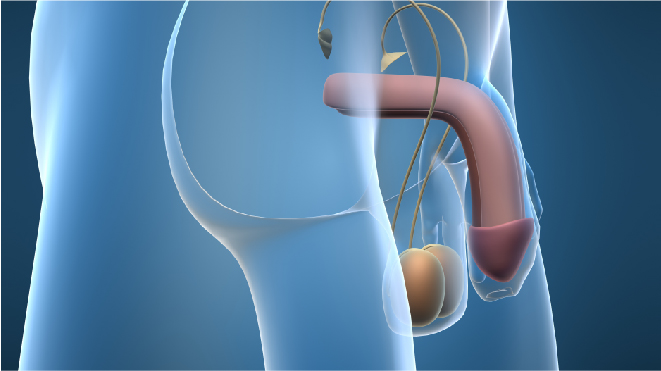
Testicular cancer is the cancer in the testicles, the male reproductive organ that makes hormones and sperm. To learn more about testicular cancer, read here.
What is prognosis?
Prognosis is a medical term for predicting the expected development of a disease and it includes whether the signs and symptoms will improve, worsen or remain stable over time and the time period of the same. It also covers expectations of quality of life such as the ability to carry out daily chores, the potential for complications and associated health issues, and also the likelihood of survival.
What are the factors that affect the prognosis of testicular cancer?
The following are some of the important factors to consider to pick a treatment plan and determine the patient’s prognosis:
Type of testicular cancer:
The type of testicular cancer plays an important role to determine the prognosis and treatment options as the speed of growth and spreading of the testicular cancer depends on the cancer type.
Stage:
The stage of cancer is an important parameter because the extent to which the testicular cancer has spread and the body organs affected determines the course of action and the chances of recovery.
Overall health:
The overall health, medical history and the patient’s response to treatment helps decide the treatment methods and their susceptibility to complications.
Age:
The age of the patient is an important factor to decide the treatment as the doctors have to consider the side effects associated with the treatment and how it affects the patient.
Prognosis for testicular cancer:
The survival rate of testicular cancer is higher than many other cancer. Regular follow-up and review is a major factor in ensuring good outcomes, so it’s important that one attends
all follow-up appointments. Testicular tumors are divided into three groups, based on how well the tumors are expected to respond to treatment of the testicular cancer.
Good prognosis:
For non seminomas, if the tumour is found only in the testicle or in the retroperitoneum, the area outside or behind the abdominal wall, or the tumour has not spread to organs other than the lungs and the levels of all the tumour markers are slightly above normal, it is called a good prognosis and the patient has a high chance of continuing life comfortably post treatment.
For seminoma, it is good prognosis if the tumor has not spread to organs other than the lungs and the level of alpha-fetoprotein (AFP) is normal. The levels of Beta-human chorionic gonadotropin (β-hCG) and lactate dehydrogenase (LDH) can be at any level .
Intermediate prognosis:
For non seminoma, if the tumour is found in one testicle only or in the retroperitoneum and has not spread to organs other than the lungs and if the level of tumour markers are above normal but in the intermediate range (not in the range of bad prognosis risk), it is called intermediate prognosis.
For seminoma, the tumor has spread to organs other than the lungs and the level of AFP in blood is normal while β-hCG and LDH can be at any level, it is intermediate prognosis.
Bad prognosis:
If the level of tumour markers is high and/or the testicular cancer has spread to other organs other than lungs, it is bad prognosis for non seminomas
Seminomas do not have poor prognosis group.
Treatment of testicular cancer:
The following is the overview of testicular cancer treatment:
Surgery:
Surgery is one of the best methods of treating testicular cancer and can completely eliminate cancer in the early stages and even if the testicular cancer has metastasized, it is essential to remove one or both the testicles if the cancer has affected both. Radical inguinal orchiectomy and retroperitoneal lymph node dissection are the two major surgeries for testicular cancer treatment. Read more about surgery for testicular cancer here.
Chemotherapy:
Chemotherapy uses drugs to kill cancer cells throughout the body and is used if the testicular cancer has metastasized to other organs or if there is a chance of recurrence. It can be used both before the surgery and after as an adjuvant therapy. Read more about chemotherapy for testicular cancer here.
Radiotherapy:
Radiotherapy involves killing cancer cells using high intensity radiation and is also used if the tumours are to be targeted unlike chemotherapy which kills cancer cells in all body parts, however due the risk of radiotherapy to cause infertility, it is used only in case the cancer has spread or can recur. Read more about radiotherapy for testicular cancer here.