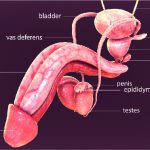
Testicular cancer is the cancer in the testicles, the male reproductive organ that makes hormones and sperm. To learn more about testicular cancer, read here.
How radiation therapy works for testicular cancer:
This therapy uses high energy X-rays to destroy the testicular cancers. Radiation is given to the patients under strict monitored doses to control the growth of the cancerous cells. It is mainly used in treating metastasized testicular cancers. It is often given before/after surgeries or combines with chemotherapy. The main benefit of this treatment is that is does not just kill the cancer cells but also helps in reducing pain and other symptoms of the cancer. Read more about the symptoms of testicular cancer here.
How is radiation therapy given:
If the radiation is externally given, a machine called the linear accelerator is used, whereas a radioactive isotope is placed in the patient’s body when the radiation is given internally.
In almost all cases of testicular cancer, external beam radiation is used. Radiotherapy is also given post surgery in the treatment of seminomas to prevent the recurrence or metastasizing of cancer.
Types of radiation therapy for testicular cancer
Radiation to treat the testicular cancer cells aims mainly at the testes along with the lymph nodes in the abdomen and pelvis. Following are the types of radiation therapies used for treating testicular cancer:
External beam radiation therapy (EBRT):
External beam radiation therapy aims at killing the cancerous tissues in the body by direct a beam of radiation externally using an X ray machine called the linear accelerator. In treating testicular cancer, it is used in shrinking the tumours and killing the cancer that has spread to the lymph nodes and other parts of the body.
During EBRT, the machine projects beams of radiation on the areas where there is a presence of tumours or cancer cells. The machine moves around the person and delivers the radiation in all possible angles and directions. Higher and more accurate doses are given in order to avoid the side effects caused by damaging the healthy blood cells.
Intensity modulated radiation therapy (IMRT):
IMRT is a treatment using for recurring testicular cancer, the procedure includes delivering the radiation externally using the linear accelerator. But in this treatment, the accelerator delivers radiation in directions and angles that actually match the 3D geometrical shape of the tumour. Accurate and high doses of radiation are given to the patients who have not been completely cured with lower doses. The advantage of this treatment is that because of precision accuracy, it reduces the healthy cells being exposed to the radiation.
Tomotherapy:
This treatment involves a machine which is a combination of intensity modulated radiation therapy (IMRT) and the computed tomography (CT) scan. This machine is highly advanced and can help deliver radiation to tumours with complex shapes. The CT scan confirms the shape, size and position of the tumour and tomotherapy reduces the exposure to healthy tissues and organs.
Side effects of radiation therapy:
Side effects occur due to the damage of the healthy blood cells in the body, when the radiation is given in high doses, it may have adverse effects on the body. The short term side effects go away after one to two weeks of treatment, but the patient has to deal with the long term side effects for considerably very long time. On noticing any adverse side effects, doctors have to consulted immediately. Side effects of radiotherapy in treating testicular cancer could be:
- Skin peeling and blistering in the radiated areas (rare)
- Nausea
- Vomiting
- Diarrhea
- Fatigue
- Loss of appetite and weight loss
- Makes the patient prone to infections (due to lower white blood cell count)
- Anemia (due to lower red blood cell count)
- Difficulty in blood clotting, easy bleeding and bruising (caused due of low platelet count)
- Soreness and swelling
- Bladder problems
Long term side effects of radiation in treating testicular cancer:
- Damage to blood vessels: High doses of radiation kills the healthy blood vessels and drops the blood count.
- Effect on kidneys: Radiotherapy when aimed near the kidneys can cause renal failure, a state in which the kidneys are not capable of filtering waste from the body.
- Effect of heart: High doses of radiation leads to increased blood pressure and disturbances in the heart rhythm, which increase the risk of cardiovascular diseases.
- Hormonal imbalances: Radiation therapy is sometimes given with chemotherapy in patients who need higher dosage. This causes an imbalance in the testosterone levels in the body.
- Developing other cancers: Men who had radiation for testicular cancer are prone to develop other cancers in the regions exposed to radiation.
- Infertility: When the radiation is applied to the testicles or near that region, it could lead to a poor production of sperm in the long run.
Dosage and survival rate:
The doses of radiation purely depends on the type and stage of testicular cancer, the patient has to share all this previous medical record along with useful medical information, which would help the doctor set a proper dose for the patient.
Generally, 2500 rads is given for 15 to 20 days for stage I seminomas. The same is given for stage II seminomas as well, with an extra 1000 rads aimed at the enlarged lymph nodes. Radiotherapy in the treatment of testicular cancer has a good survival rate but is not the most preferred course of action as the radiation can can adverse side effects like infertility. Increasing the dosage of radiation and giving it the right way without majorly affecting other parts of the body increases the survival rate of radiation therapy for testicular cancer.
After care:
Post any treatment for cancer, it is very important to that the patients maintain a proper follow up and a healthy regime. Know more about the follow care for testicular cancer here. The following are a few aftercare tips for the patients:
- Skin should always be moisturized to reduce peeling and dryness
- Have nutritious meals
- Stay hydrated all day
- Maintain proper weight
- Depending on your energy levels, minimum basic exercise is required.
- Regular monitoring of blood cell count
- Stay in regular touch with the health care
- Infusion of blood or hormones may be required in a few cases
- In case of any adverse side effects, doctors have to be consulted immediately
- Special care is required to shield the other body parts and especially the testicles to preserve infertility