Dr Sumant Gupta, Head of Department and Senior Consultant at Sarvodya Cancer Institute, gives an overview of how leukemia is currently treated.
Leukemia is a broad term for cancers that begin in the bone marrow, which produces blood cells. Bone marrow is a soft, spongy tissue inside the bones and contains hematopoietic stem cells which are immature cells that can develop into the blood cells: red blood cells (RBC), white blood cells (WBC) and platelets.
When the cells in the bone marrow undergo any mutation, they start multiplying into abnormal cells. These cells, called leukemia cells, divide and grow uncontrollably. Over time, they will crowd out or suppress the marrow’s ability to produce enough healthy blood cells.
Leukemia cells are usually immature white blood cells, which are functionally incapable. In patients with leukemia, there will be a rapid increase in abnormal white blood cells.
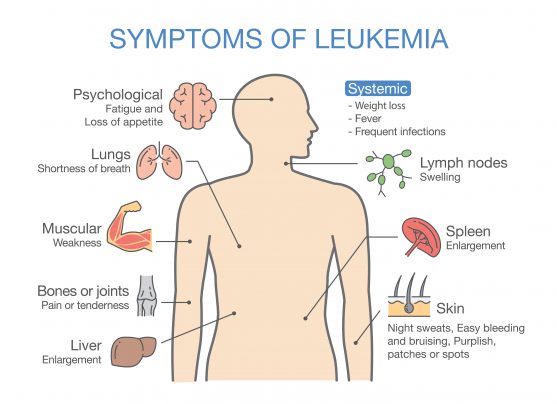
Signs and symptoms of leukemia
The most common signs and symptoms of leukemia are:
- Unexplained fever
- Headaches
- Bruising /bleeding
- Fatigue
- Joint pain
- Frequent infections
- Enlarged lymph nodes
- Unintentional weight loss
- Night sweats
- Shortness of breath
Risk Factors for leukemia
Factors that may increases your risk of developing leukemia includes:
- Previous cancer treatment
- Family history of leukemia
- Genetic disorders such as neurofibromatosis, Bloom syndrome, Shwachman-Diamond syndrome, Down Syndrome.
- Long-term exposure to certain chemicals, such as gasoline, benzene, formaldehyde.
- History of smoking
Diagnosis of leukemia
The diagnosis is based on the signs and symptoms, patient’s medical history, and family history. Unlike other cancers, leukemia cells generally cannot be visualized using imaging tests, such as X-rays.
Specific diagnostic tests may be advised, if leukemia is suspected:
-
Complete blood count (CBC)
The levels of blood components such as red or white blood cells or platelets are evaluated. Abnormal levels of blood components indicate leukemia.
-
Bone marrow aspiration
This test is recommended if the blood test shows unusual blood counts or immature cells. In this procedure, a sample of the fluid part of bone marrow is taken with a needle and analysed for the presence of leukemia.
-
Bone marrow biopsy
The biopsy is done under the influence of a local anaesthetic or a sedative. In this procedure, a small sample of tissue from the bone marrow or the lymph nodes is removed using a sterilized needle, and the type and growth rate of leukemia is evaluated.
-
Spinal tap
A spinal tap or lumbar puncture is used to analyse the spread of leukemia to the cerebrospinal fluid (CSF).
Types of leukemia
Leukemia can be classified based on how quickly the disease progresses and by the type of blood cell involved.
Based on the rate of cell division and disease progression, leukemia can be of two types:
Acute leukemia is a rapidly progressing cancer, and chronic leukemia usually progresses more slowly. Acute leukemia is common among children while chronic leukemia is more commonly seen in adults.
Based on the origin of cancer and the type of blood cell involved, leukemia is divided into four types, they are:
-
Acute myeloid leukemia (AML)
This cancer involves rapid growth of abnormal myeloid cells (cells in the bone marrow which can become red blood cells, white blood cells, or platelets), which move into the bloodstream and spread to other parts of the body. AML is more common in older adults.
-
Chronic myeloid leukemia (CML)
This is a slow-progressing leukemia that originates due to genetic changes in the myeloid cells. Over time, it spreads to the blood and to other parts of the body. This type of leukemia is rare. Adults are more likely to develop CML than children
-
Acute lymphoblastic leukemia (ALL)
ALL usually develops due to some abnormalities in the DNA of bone marrow, and is more common in children. It begins in the immature white blood cells, B or T lymphocytes. ALL can affect the bone marrow all over the body.
-
Chronic lymphocytic leukemia (CLL)
This type of leukemia begins in lymphoid blood cells of the bone marrow and affects the white blood cells. The abnormal blood cells accumulate in the body making it difficult for the body to fight infection. It may also spread to lymph nodes and organs like liver and spleen. CLL is rare in children and usually affects older adults.
Stages of leukemia
Identifying the stages of leukemia helps to determine how far the cancer has spread. The evaluation of progression of the condition can help physicians to determine the most appropriate treatments.
Chronic leukemia is staged using the Rai system. It considers the number of lymphocytes in the blood, the presence of anemia or thrombocytopenia and the degree of enlargement of lymph nodes, spleen or liver.
Acute leukemia is staged and classified histologically based on the French-American-British (FAB) system. This takes into account the number of healthy blood cells, the size and number of the leukemia cells, the chromosomal changes of the leukemia cells and other genetic abnormalities.
Treatment of leukemia
The treatment options depend on the type of leukemia, age and overall health, and extent of spread of leukemia to other organs or tissues. The treatment team will discuss the treatment options, its benefits, possible risks and side effects.
There are five common treatment categories available for leukemia. They include:
Chemotherapy
Chemotherapy involves periodic administration of anti-cancer drugs, often over the course of several months. This is the main treatment for almost all kinds of leukemia. It aims for cure, control and palliation of leukemia. The drugs are typically given orally, usually in the pill form or intravenously (directly into the vein). The treatment is planned as cycles in which a few days of rest are allowed for the body to recover before the next cycle. The duration of treatment can vary from six months to indefinite treatment.
Chemotherapy treatment is typically divided into 3 phases:
- Induction phase: This is a short and intensive phase, lasting about a month. The drugs given during this phase destroy the cancer cells in the blood and bone marrow.
- Consolidation (intensification) phase: During this phase, that usually lasts for a few months, the drugs are given to destroy the cancerous cells that may remain after the induction phase.
- Maintenance (post-consolidation) phase: This is the final phase that typically lasts for about 2 years. Low dose drugs are given to prevent the recurrence of cancer.
Usually, a combination of chemotherapy drugs are used, for example, a combination of an anthracycline, doxorubicin or idarubicin and cytarabine, or combination of Venetoclax with azacitidine or decitabine or low-dose cytarabine, etc.
Side effects of Chemotherapy
Chemotherapy can cause side effects depending on the dose of medication and the intensity of therapy. The side effects are different for each patient. Some of the common side effects of chemotherapy include:
- Nausea and vomiting
- Loss of appetite
- Hair loss
- Mouth sores
- Diarrhea or constipation
- Fatigue
Targeted therapy
Targeted therapy for leukemia acts by targeting the proteins that control how cancer cells grow, divide, and spread. This therapy identifies and attacks specific cancerous cells without causing much harm to the normal cells. Examples of targeted therapy include:
- Monoclonal antibodies (such as inotuzumab, gemtuzumab, rituximab, ofatumumab, obinutuzumab, alemtuzumab)
- Tyrosine kinase inhibitors (such as dasatinib, nilotinib, ponatinib, ruxolitinib, fedratinib, gilteritinib, midostaurin, ivositinib, ibrutinib, venetoclax).
The common side effects associated with targeted therapy include:
- Skin irritations and acne like eruptions.
- Blood clotting and wound healing problems
- Nausea and vomiting
- Fluctuating blood pressure
Stem-cell transplantation
In this treatment, the diseased bone marrow is replaced with a new healthy bone marrow. These healthy cells are taken from the patient (autologous transplants) or from a donor (allogeneic transplants) and are infused back into the patient. These healthy hematopoietic stem cells will grow and multiply forming new blood cells that develop into all the other types of cells your body needs.
Before undergoing stem-cell transplantation patients are advised to undergo chemotherapy or radiation therapy for destroying the damaged bone marrow.
The possible side effects of stem-cell transplantation are:
- Mouth and throat pain
- Bleeding and transfusions
- Nausea and vomiting
- Graft-versus-host disease
- Interstitial pneumonitis and other lung problems
- Infections