How is throat cancer diagnosed?
It is important to diagnose throat cancer as early and accurately as possible. An accurate diagnosis helps to increase the chances of successful treatment and recovery for throat cancer patients. An early diagnosis can also determine the extent of organ-preserving procedures with which a patient can retain the ability to speak and swallow after the completion of treatment. Oncologists are supposed to ask questions about the patient’s general health, their lifestyle habits (such as smoking or drinking), their sexual history; and their family’s medical history or history of familial cancer.
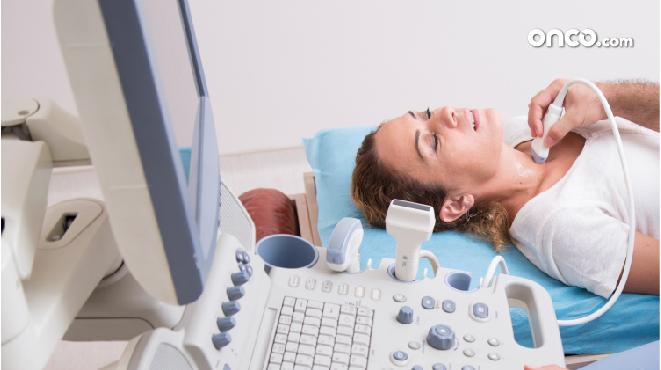
If a patient presents with symptoms of throat cancer, the following tests are recommended to confirm the diagnosis:
Clinical Examination and Endoscopy
A clinical examination by an ENT surgeon helps to discover the cancerous lesions. Endoscopy involves using a scope to take a closer look at the throat. Oncologists can use a special lighted scope fitted with a tiny camera (known as an endoscope) to transmit images on to a video screen that monitors for signs of abnormalities or malignant growth. The endoscope can be inserted either through the mouth or through the nose. The endoscope also contains a biopsy forcep that can remove tissue samples to proceed with a biopsy if the monitor shows a visible abnormality.
In certain cases where a patient exhibits difficulty in swallowing, a fiberoptic endoscopic examination of swallowing (FEES) may be performed. In such cases, a small, flexible endoscope is inserted through the nose to examine the constrictions that prevent a patient from swallowing food on a normal basis. A barium swallow X-ray may also be used in such scenarios.
Imaging tests
Aside from the confirmatory diagnostic tests, the following types of imaging tests are also used to check for signs of abnormalities before a deeper investigation can be ordered:
- Chest X-rays
- CT or CAT (computed axial tomography) scans of the upper body
- PET (positron emission tomography) CT scans of the upper body
- MRI (magnetic resonance imaging) scans of the neck region
Biopsy
In a biopsy, surgeons remove a small tissue sample from the tumour/cancerous ulcer and test it for abnormalities. Once a tissue sample has been extracted, a histopathologist studies the sample under a microscope to detect the presence of malignant (rapidly dividing, cancerous) cells. There are two types of biopsies used in the diagnosis of throat cancer:
Conventional biopsy (incisional/punch): This is the most commonly practised type of biopsy. In such a process, oncological surgeons remove a very small part of the tissue area where cancer is suspected to have developed.
Fine-needle-aspiration biopsy (FNAC): FNAC biopsies are used in case of visible lumps in the neck. In an FNAC biopsy, a thin needle is inserted into the affected area, and then a tissue sample is withdrawn and examined under a microscope.