Skin changes are quite common among cancer patients undergoing chemotherapy. In most cases, the skin changes are not severe, but can be noticeable and uncomfortable. This reminds the patients of their cancer battle and affects their mental health.
Sometimes, these changes in the skin can affect the treatment plan and be detrimental to the patient’s quality of life. However, the good news is that most skin changes are manageable and reversible after completion of treatment.
Why does chemotherapy affect the skin?
Chemotherapy focuses on one feature of the cancer cells – they divide at a faster rate than the normal cells. Thus, the drugs target the fast-growing cancer cells. This is the basic principle for many chemotherapy agents.
However, this mechanism of action can affect the normal fast-growing cells of the body, such as the skin, hair follicles and cells lining the digestive tract. This results in side effects such as changes in the skin, hair loss, and diarrhea and other gastrointestinal problems.
Which chemo drugs cause skin changes?
There are several skin changes that occur as a side effect of chemotherapy. The side effect depends on the drugs administered. The most common ones are discussed below.
Skin Rashes
A skin rash is a common side effect of chemotherapy. It can appear on the face, scalp, neck, upper back, chest, and other parts of the body. These rashes can be itchy, painful or lead to a burning sensation.
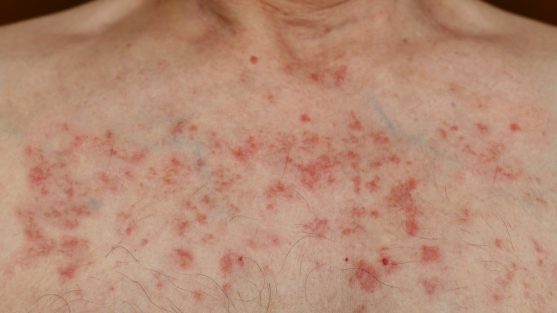
Some of the common drugs that can cause skin rash include, taxanes such as paclitaxel and docetaxel, gemcitabine, oxaliplatin and bleomycin.
How can I manage my skin rashes?
- Your team of doctors may recommend some lotions, mild soaps, and moisturizers, to help manage the rash.
- In case the rash doesn’t get better, your doctor may prescribe a steroid cream, along with antibiotic creams or oral antibiotics.
- For severe rashes, your doctor may prescribe oral steroids as well as a steroid cream.
- If required, your doctor may stop your chemotherapy for a short-term and resume at a lower dose.
Here are some things you can do to reduce your rashes:
- Use a soft cloth, warm water and gentle soap to clean the affected area.
- Moisturize your skin regularly.
- Do not expose the affected region to extreme heat or cold conditions.
- Wear soft, comfortable, loose fitting clothes.
- Avoid direct sun exposure as much as possible, it may trigger or worsen the rash.
- Wear clothes that cover all your skin, while stepping out in the sun.
- Use a broad-spectrum sunscreen with SPF 30 or more one hour before stepping out.

Moisturising can ease rashes
Extravasation and Desquamation
Most chemotherapy drugs are administered via intravenous infusions. Occasionally, the drug may accidentally leak outside the vein, into the surrounding tissues. This is known as chemotherapy extravasation.
This can cause pain and burning sensation. If left untreated, it may result in an open wound. Based on the type of drug infused, this can cause serious complications in patients.
However, quick detection of extravasation and treatment can reduce the tissue damage.
These steps are taken to reduce the tissue damage:
- Immediate stopping of chemotherapy infusion
- Hot or cold compress
- Antidotes based on drug type may be administered
Most extravasation incidences can be prevented with careful monitoring by the health care team, including regular inspection of the intravenous access site, flushing the access before and after the infusion, and patient monitoring during the infusion.
Hand and Foot Syndrome
If you develop hand and foot syndrome, the skin on the palms and soles of your feet may become red, sore, and may peel (desquamation).
Other symptoms include:
- pain
- numbness
- dryness
- burning and/or tingling sensation
- sensitivity to touch
- tightness of the skin
- blisters
Hand and foot syndrome may make simple tasks difficult and affect your quality of life.
Some drugs that are more likely to cause hand and foot syndrome include docetaxel, paclitaxel, cytarabine, capecitabine, doxorubicin, floxuridine, fluorouracil, idarubicin, liposomal doxorubicin, vemurafenib, etc.
How can I manage hand and foot syndrome?
- Topical or oral pain relievers, such as lidocaine, naproxen, ibuprofen, or celecoxib, may help relieve pain.
- Topical moisturizing exfoliant creams, especially those containing salicylic acid, urea, or ammonium lactate, can also be recommended.
- Ice packs placed under the hands and feet while receiving chemotherapy can also prevent hand and foot syndrome.
Given below are some tips and instructions that can help you relieve the symptoms and manage hand and foot syndrome:
- Avoid using hot water on your hands and feet.
- Take showers or baths using cold water.
- Gently pat your skin dry after bathing or washing.
- Use a wet towel, ice packs, or place your hands and feet under cold running water for 15 to 20 minutes to cool them. Do not apply ice directly to the skin.
- Avoid sitting in the sun or in front of a sunny window.
- Do not indulge in activities that involve rubbing your hands or feet, such as aerobics, jogging, and racquet sports.
- Stay away from harsh chemicals present in household cleaning products or laundry detergents.
- Avoid using tools that have a hard surface such as knives, garden tools, and screw drivers.
- Apply skin care creams and moisturizers gently, without rubbing or massaging with force.
- Wear comfortable, loose fitting, well-ventilated clothes.
- Use thick socks and soft slippers to reduce friction while walking.

Ice packs can ease symptoms
Dry and itchy skin
Dry skin can be rough, red, flaky, may have cracks in the skin, and at times painful.
Prolonged itching may lead to breaking of the skin, bleeding, or infection.
How can I manage dry and itchy skin?
- Mild dry skin can be managed with topical emollients (liquid or cream).
- Severe cases may require use of topical corticosteroids.
- Your doctor may prescribe oral antihistamines or topical steroids to manage itchy skin.
The following tips may help manage dry and itchy skin:
- Use warm water for showers and baths, extreme hot water can cause more dryness.
- Use moisturizers that contain urea, lactic acid and salicylic acid, or the ones recommended by your doctor.
- Apply a moisturizing cream two times a day and within 15 minutes of showering.
- Do not use products that can irritate the skin, including soaps, fragrant creams, detergents, etc.
- Do not rub your skin. Use a clean soft towel to pat your skin dry.
- Choose an electric razor over a blade, to avoid cuts and irritation.
- Keep your room cool, and keep it well-ventilated.
- Wear comfortable, loose-fitting, soft clothes.
- Keep yourself hydrated by drinking enough water and other fluids.

Drinking water can reduce itchy skin
Hyperpigmentation
Hyperpigmentation means darkening of the skin. This can occur over a small region or at one particular spot.
It usually occurs within two to three weeks of initiation of chemotherapy and resolves 10 to 12 weeks after stopping treatment.
Drugs such as cyclophosphamide, 5-fluorouracil, methotrexate and busulfan, have shown to cause hyperpigmentation.
Photosensitivity
Photosensitivity, or sensitivity to light, can also be a side effect of chemotherapy.
One of the chemotherapy drugs that causes sensitivity to light is 5-fluorouracil.
How can I manage photosensitivity?
Given below are some tips to treat and prevent photosensitivity caused by chemotherapy:
- Limit direct sun exposure.
- Cover your whole body with clothes and use a hat, while stepping out in the sun, particularly between 10 AM and 4 PM.
- Use a broad-spectrum sunscreen with at least SPF 15, before going out.
- Reapply your sunscreen every 2 hours or every hour if you are sweating or swimming.
The skin changes mentioned above may or may not occur in all patients undergoing chemotherapy.
While the home care measures listed in this article may help you manage your skin changes, it is always advisable to consult your doctor before implementing any of these measures.
Moreover, your doctor may recommend some further tips and guidelines to manage your specific skin problems.

