What is chemotherapy for breast cancer?
Chemotherapy refers to the administration of drugs to destroy cancer cells. Usually, chemotherapy drugs identify cells to be cancerous based on their ability to divide fast, rapidly. These drugs attack the growth and divisive ability of such cells, killing them in the process. Medical oncologists are involved in prescribing a chemotherapy regimen for breast cancer patients. Chemotherapy for breast cancer is a part of systemic treatments used for breast cancer.
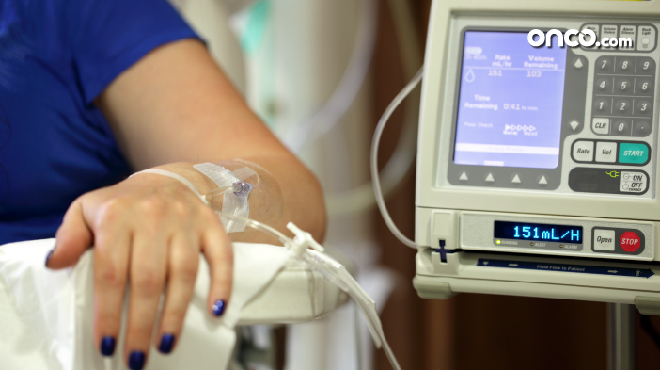
While the most common way to give chemotherapy is an intravenous (IV) tube, it can also be delivered using a needle, an injection under the skin, into a muscle, or as a pill or capsule (oral chemotherapy).
What is neoadjuvant chemotherapy?
Neoadjuvant chemotherapy refers to cancer treatment that is before surgery to shrink the size of the tumor and make it easier to remove.
What are the advantages of neoadjuvant chemotherapy?
Neoadjuvant therapy has many advantages, including:
- Potential candidates for mastectomy (breast removal) reduces their tumor size and then go for lumpectomy (breast conservation).
- Surgery becomes easier to perform.
- Oncologists and multidisciplinary teams have a better idea of the patient’s response to different cancer-specific medicines
- Patients can enroll in relevant clinical trials before surgery.
What is adjuvant chemotherapy?
When chemotherapy is given after surgery to remove microscopic cancer traces and reduce the risk of recurrence, it is adjuvant chemotherapy.
Chemotherapy schedule for breast cancer
For breast cancer, a chemotherapy schedule consists of a specific number of cycles over a set period, and then periodically with gaps. Chemotherapy can be administered on different schedules, depending on has proven to work best in the past, or during research, or during clinical trials that have been conducted for that specific type of drug or regimen.
Usually, chemotherapy cycles are organized either once a week, once every two weeks, once every three weeks, or even once every four weeks.
Chemotherapy drugs used in the treatment of breast cancer
For treating breast cancer, a patient can receive either one drug at a time or a combination of different drugs, administered on the same schedule/regimen. The most common drugs used for chemotherapy treatments in breast cancer include:
- Capecitabine
- Carboplatin
- Cisplatin
- Cyclophosphamide
- Docetaxel
- Doxorubicin
- Pegylated liposomal doxorubicin
- Epirubicin
- Fluorouracil
- Gemcitabine
- Methotrexate
- Paclitaxel
- Protein-bound paclitaxel
- Vinorelbine
- Eribulin
- Ixabepilone
Side effects of chemotherapy in the treatment of breast cancer
Since chemotherapy does not discriminate between cancer cells and other rapidly dividing healthy cells, it often ends up targeting and killing cells that are involved in regular bodily functions, leading to one or many severe side effects. Doctors advise tertiary treatment or precautions for some of these side effects, but patients must to stay on guard for symptoms arising due to chemotherapy, such as:
- Persistent fatigue
- Hair loss (partial or complete)
- Susceptibility to easy bruising and bleeding
- Low white blood cell (WBC) count, which may lead to infections
- A drop in red blood cell (RBC) counts, leading to anemia
- Nausea and vomiting
- Loss of appetite and weight loss
- Constipation, diarrhea
- Mouth, tongue, and throat problems (such as sores and blisters)
- Pain in swallowing food
- Nerve numbness, tingling, and pain
- Muscle pain and numbness
- Dry skin
- Change of color of the nails
- Bladder changes, kidney problems
- Urinary incontinence
- Reduced concentration and focus (sometimes called ‘Chemo brain’)
- Frequent, inexplicable mood changes
- Loss of libido and sexual function
- Fertility problems
Side effects of chemotherapy in breast cancer treatment
Chemotherapy is one of the most common systemic therapies in breast cancer treatment. It is given in adjuvant, neoadjuvant and palliative settings. Due to the non-targeted nature of chemotherapy drugs, they often target healthy living cells, which are rapidly dividing cells, leading to multiple side effects. Some of these side effects become very prominent in breast cancer patients. The side effects of chemotherapy can either be acute side effects or late side effects
Fatigue
Fatigue is one of the most common side effects of chemotherapy in breast cancer treatment. Almost 9 out of 10 people undergoing chemotherapy experience some form of fatigue (moderate to severe) during treatment. Some factors that can lead to this type of fatigue are anemia and vasomotor symptoms, which can lead to sleep disturbance and depression. For most patients, the cause of fatigue remains unknown, and they should be treated symptomatically. However, in most cases, post-treatment fatigue resolves after the treatment finishes.
Hair loss and other hair changes
Chemotherapy drugs treat cancer by destroying all cells within the living body that are dividing rapidly. In doing so, they also target cells within hair follicles, and as a result, patient can experience mild to severe hair loss, hair thinning, or change in the color of hair. Hair thinning typically begins after the second or third cycle of chemotherapy. Hair loss due to chemotherapy is temporary, and regrowth of hair begins after the completion of treatment.
Diarrhea
Diarrhea is a condition where patients experience loss of bowel control, with loose or watery stools more than three times a day. Patients also present with tertiary symptoms such as cramps, bloating, and nausea. Diarrhea can occur as a result of fluid-retention problems arising due to chemotherapy, and also as a result of infection.
Anemia
A common side effect of chemotherapy is myelosuppression, which can also lead to anemia. Anemia happens due to a drop in red blood cell count during chemotherapy cycles. Anemia can impact the patient’s general health, and can also cause fatigue. Regular monitoring of the patient’s blood-work is important during chemotherapy treatments.
Nausea and vomiting
Nausea, or a feeling of frequently wanting to throw up, is a common side effect of chemotherapy treatments. The drugs used for the treatment of breast cancer are moderate-to-high emetogenic drugs. It is possible for patients to be put on anti-emetogenic drugs, based on the chosen chemotherapy regimen.
Weight loss, loss of appetite and weight changes
Chemotherapy patients often complain of a loss of appetite and partial or severe weight loss, with anorexia. The shock of a breast cancer diagnosis, and the overall disruption of the patient’s lifestyle, including reduced physical activity and energy levels during treatment. Moreover, nausea also contributes to a loss of appetite.
Infections and myelosuppression (immune system suppression)
Chemotherapy leads to myelosuppression or a reduced count of white blood cells (WBCs) which, in turn, can lead to the patient being susceptible to a lot of infections, by allowing harmful bacteria, viruses, parasites, or fungi to enter a site in the body and reproduce freely. The immune system may not function at full capacity for breast cancer patients receiving chemotherapy, which places them at a higher risk for infections. In most patients, myelosuppression is seen 10 to 14 days after each cycle. And this usually resolves itself before the next regimen. However, if the myelosuppression is severe and persistent, it may result in fever or life-threatening infection.
Bone weakness, bone pain and breaking bones
Characterized by their growing nature, bone cells are also easy targets for chemotherapy drugs. Osteoporosis happens when the bone mass and bone density go below average, due to attack by chemotherapy drugs. Chemotherapy recipients with osteoporosis are at serious risk of breaking bones at joints near the spine, wrist, or hip.
Mouth sores and ulcers
Chemotherapy regimens disrupt the human immune system, leaving the oral cavity susceptible to yeast infections, bacterial infections, and other types of ulcers. These ulcers can become red or swollen and can affect the patient’s ability to talk, eat, drink, chew, or swallow – thus further contributing to weight loss and mood swings.
Chemo brain
‘Chemo brain’ is a common term for cancer patients and survivors who experience mood-related issues, as well as thinking and memory problems that can spring up after receiving chemotherapy. It is chemotherapy-related cognitive impairment, or cognitive dysfunction.
Skin and Nail Changes
Chemotherapy drugs can destroy rapidly growing cells found in the skin and nail tissue; which, in turn, leads to skin that is dry, itchy, patchy (red) or skin that peels easily. Some patients can develop a rash or increased sun sensitivity, leading to easy sunburns. Furthermore, nail changes due to chemotherapy can include dark, yellow, or cracked nails and red cuticles that hurt at a touch.
Fertility Changes
Chemotherapy-induced amenorrhoea is one of the common side effects. These drugs cause a variable degree of ovarian dysfunction. Furthermore, some women can develop permanent ovarian failure, while others develop temporary ovarian failure with the return of regular menstrual cycles after the treatment.